Dysautonomia Isn’t One Diagnosis — It’s a Pattern of Dysregulation
This training explains dysautonomia through a systems-based lens — focusing on nervous system regulation, metabolic stability, inflammation, hydration, and rhythm restoration.
Most conversations about dysautonomia start with the assumption that it’s a single disease — one diagnosis, one label, one fix.
But that framework doesn’t match what we see clinically.
Dysautonomia is an umbrella term. It describes a state where the autonomic nervous system — the system responsible for regulation and rhythm — has lost its ability to adapt smoothly.
When we see dysautonomia, what we are really seeing is a body that has been navigating too much for too long, without adequate recovery or resources.
So this is not a “diagnosis discussion.”
This is a regulation discussion.
It’s about understanding why the system lost regulation, and how the body restores it.
The Autonomic Nervous System Is the Body’s Master Regulator
Your autonomic nervous system governs:
Heart rate and blood pressure
Circulation and vascular tone
Digestion and gut motility
Temperature regulation
Immune signaling
Hormone release
Sleep-wake cycles
Stress response and recovery
And it is constantly responding to input from:
Food and blood sugar levels
Inflammation and immune activation
Hydration and electrolytes
Toxic load and environmental stressors
Circadian cues (light, timing, stimulation)
Perceived safety vs. threat
When the system is supported, it’s flexible, responsive, and resilient.
When it becomes overwhelmed, under-fueled, inflamed, or overstimulated, it loses regulation.
That state is what we call dysautonomia.
Dysautonomia Rarely Happens in Isolation
Clinically, dysautonomia is commonly seen alongside:
Autoimmune patterns
Mast cell activation (MCAS) / histamine intolerance
Post-viral syndromes
Chronic gut inflammation or intestinal permeability
Hormonal depletion or transition states
Longstanding stress chemistry overload
This overlap matters because it reveals something critical:
Dysautonomia is rarely the root. It’s a response pattern.
The nervous system is responding to the internal environment it is operating within.
Dysautonomia Isn’t Mysterious When You Look Through a Systems Lens
When viewed through a systems framework, dysautonomia often reflects predictable pressures of modern physiology.
Here are five of the most common:
1) Metabolic instability (blood sugar swings)
Blood sugar spikes and crashes are interpreted by the nervous system as threat.
Every crash requires compensation through:
Adrenaline
Cortisol
Sympathetic activation
Over time, this erodes nervous system flexibility and trains the system into reactivity.
2) Chronic inflammation
Inflammation interferes with:
Nerve signaling
Vascular tone
Receptor sensitivity
The nervous system becomes noisy, reactive, and inefficient.
3) The gut–immune connection
The gut and nervous system are in constant dialogue.
When the microbiome is dysregulated or the gut lining is inflamed, immune signaling can overwhelm regulation.
This is one reason so many dysautonomia cases also carry gut symptoms.
4) Hydration and electrolyte imbalance
Autonomic dysfunction often includes impaired vascular tone and signaling, which can create functional dehydration — even in people who drink plenty of fluids.
In other words: water may move through the body without being retained well at the cellular level.
5) Circadian rhythm disruption
Irregular sleep, inconsistent meal timing, overstimulation, and disrupted light exposure all degrade the rhythms your nervous system depends on.
Without rhythm, regulation breaks down.
Let’s Say This Clearly: Dysautonomia Is Not Weakness
Dysautonomia is not a character flaw.
It’s not psychological failure.
It’s not a lack of discipline.
It is biology responding intelligently to an unsustainable internal environment.
The nervous system is doing exactly what it was designed to do:
prioritize survival when conditions feel unsafe.
Why Symptom Management Alone Doesn’t Restore Regulation
Many people with dysautonomia are offered:
Heart rate control
Blood pressure support
Anxiety medications
And sometimes those tools can help reduce suffering.
But they don’t answer the real question:
Why did the nervous system lose regulation in the first place?
And without changing the underlying terrain, the system never truly regains trust.
A Systems Approach to Dysautonomia: 5 Pillars of Regulation
From a systems perspective, we don’t “fix” the nervous system.
We change the environment it is responding to.
Here are the five pillars I focus on clinically:
Pillar 1: Restore metabolic stability
The nervous system requires reliable energy.
Unstable glucose forces constant emergency signaling.
When fuel delivery becomes steady — often through a lower-glycemic, fat-supported metabolic approach — the nervous system can “stand down.”
This is not about restriction.
This is about metabolic calm.
Pillar 2: Rebuild cellular hydration
Dysautonomia often includes a state of cellular dehydration.
Electrolytes — especially sodium, potassium, and magnesium — support:
Nerve signaling
Muscle function
Vascular tone
Brain clarity
Hydration is not just water.
Hydration is electrical balance.
Pillar 3: Quiet inflammation and immune confusion
Inflammation keeps the nervous system on edge.
Reducing immune activation — especially gut-driven immune activation — is foundational.
This often includes:
Removing inflammatory food triggers
Simplifying digestion
Emphasizing soft, warm, nutrient-dense foods
Addressing dysbiosis / microbial overgrowth
When the immune system quiets down, regulation improves.
Pillar 4: Restore circadian rhythm
The autonomic nervous system runs on rhythm.
Consistent:
Wake times
Meal times
Light exposure
Rest periods
…are not “lifestyle tips.”
They are biological instructions.
Without rhythm, healing stalls.
Pillar 5: Repair the nervous system over time
Nervous system repair requires:
Fat and cholesterol
Specific B vitamins and minerals
Containment, rest, and pacing
Reduced overstimulation
Time
Repair does not happen under constant strain.
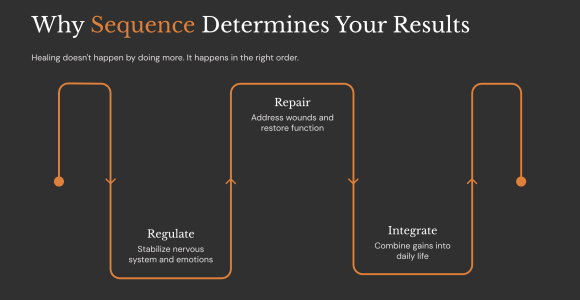
This is why sequencing matters.
The Truth About Recovery: Not Everyone Is Ready for the Same Intervention
One of the most important truths about dysautonomia is this:
Not everyone is ready for the same intervention at the same time.
So we prioritize the basics first:
safety
fuel stability
hydration and electrolytes
inflammation reduction
rhythm restoration
Healing here is not about speed.
It’s about restoring trust between the body and the nervous system.
A Different Way to Hear This Diagnosis
If you’ve been told you have dysautonomia, I want you to hold this differently:
This is not a permanent identity.
It’s not a dead end.
It’s a signal.
A signal that the system needs different conditions.
And systems can change.
Systems can regenerate.
The goal is not to force the body into performance.
The goal is to create conditions where regulation becomes possible again.
When fuel becomes stable, inflammation quiets down, hydration improves, and rhythm returns…
the nervous system remembers what to do.
And that’s the medicine.