Over the last several years, a new metabolic pattern has emerged in people following low-carbohydrate and ketogenic diets. Some individuals who improve their metabolic health dramatically—losing weight, stabilizing blood sugar, and reducing inflammation—are surprised to see one lab marker rise sharply:
LDL cholesterol.
For many people, LDL drops when metabolic health improves. But for a subset of individuals—particularly those who are lean and metabolically flexible—LDL can rise significantly, sometimes to levels above 200 mg/dL.
This pattern has come to be known as the Lean Mass Hyper-Responder (LMHR) phenotype.
For patients and clinicians alike, it raises an important question:
How should we interpret high LDL in someone who otherwise appears metabolically healthy?
Understanding the LMHR pattern requires stepping back and looking at the broader metabolic system—how the body moves fuel, how hormones regulate energy delivery, and how lipoproteins function in the bloodstream.
What Is a Lean Mass Hyper-Responder?
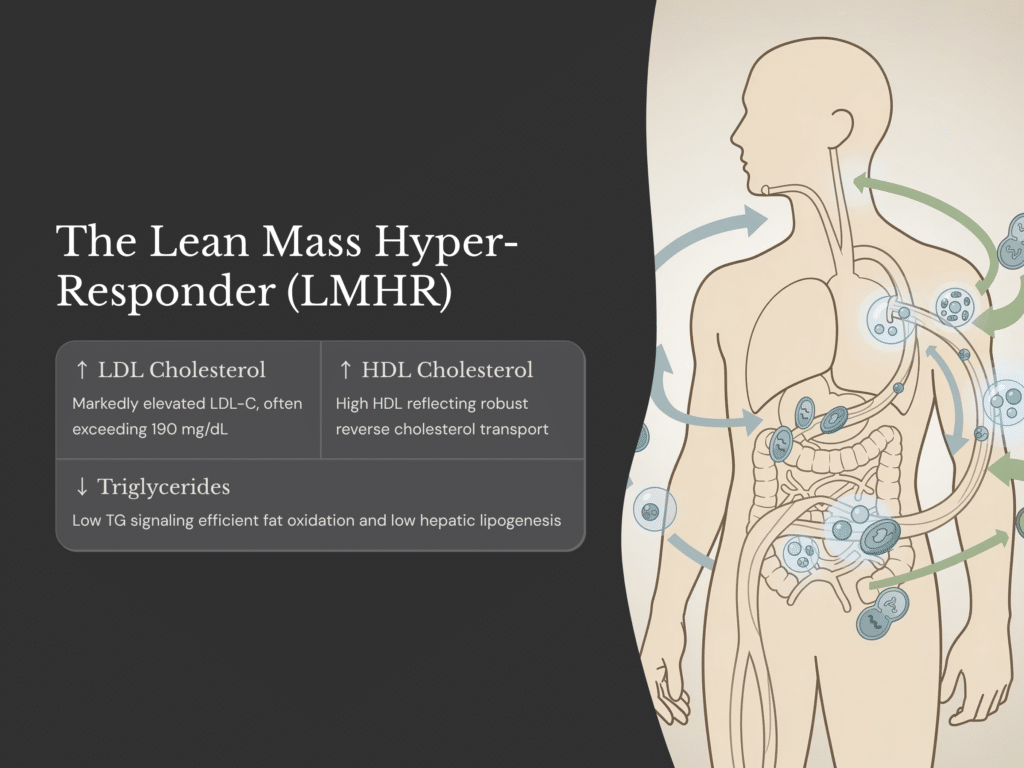
The Lean Mass Hyper-Responder phenotype was first described by researchers and citizen scientists studying lipid responses to ketogenic diets. Individuals fitting this profile tend to display three distinctive markers on a lipid panel:
• High LDL cholesterol (often above 200 mg/dL)
• High HDL cholesterol (usually above 60–80 mg/dL)
• Low triglycerides (typically below 70–100 mg/dL)
This pattern often appears in people who are:
- lean
- physically active
- metabolically healthy
- eating a low-carbohydrate or ketogenic diet
In many cases, these individuals also have excellent markers for metabolic health:
- normal blood sugar
- low fasting insulin
- low triglycerides
- high HDL
- healthy blood pressure
In other words, they appear metabolically healthy by most measures—yet their LDL cholesterol rises dramatically.
The Traditional Interpretation of LDL
For decades, LDL cholesterol has been interpreted primarily through the lens of the lipid-heart hypothesis, which suggests that higher LDL levels increase the risk of cardiovascular disease.
In that model:
Higher LDL → more cholesterol deposited in arteries → increased risk of plaque formation.
This framework has shaped mainstream medical practice for many years.
However, emerging research in metabolic health suggests that LDL levels can be influenced by how the body is transporting energy, not just by disease processes.
This is where the Lean Mass Hyper-Responder model becomes relevant.
The Lipid Energy Model
To understand LMHR physiology, we need to examine what lipoproteins actually do.
Cholesterol does not float freely in the bloodstream. Instead, it travels inside particles called lipoproteins, which also carry triglycerides and other fats.
These particles serve an important purpose: transporting energy throughout the body.
The liver packages fats into lipoproteins known as VLDL particles (very-low-density lipoproteins). These particles carry triglycerides to tissues where they can be used as fuel.
As VLDL particles deliver triglycerides to muscles and other tissues, they shrink and eventually become LDL particles.
In other words:
LDL particles are often the end stage of fat delivery in the bloodstream.
This is where the lipid energy model becomes important.
In individuals who rely heavily on fat for fuel—such as those following ketogenic diets—the body may increase lipoprotein circulation to transport fatty acids more efficiently.
The result can be:
• increased LDL particles
• low triglycerides
• high HDL
Exactly the pattern seen in LMHR individuals.
Why Lean People Show This Pattern
Interestingly, this lipid pattern tends to appear most strongly in individuals who are lean and insulin sensitive.
Why?
When body fat is low and insulin levels are low, the body often relies more heavily on circulating fats as fuel.
Instead of storing excess energy in adipose tissue, the body transports energy through the bloodstream so tissues can access it.
This process increases:
- fatty acid mobilization from fat tissue
- VLDL production by the liver
- LDL particles circulating in the bloodstream
In this context, LDL particles may function as part of the body’s fuel delivery system rather than simply a marker of lipid accumulation.
The Role of Insulin
Insulin is one of the key hormones regulating fat metabolism.
When insulin levels are high:
- fat storage increases
- fat release from adipose tissue decreases
When insulin levels are low:
- fat release increases
- fatty acids circulate more freely
- the liver packages more fats into lipoproteins
Many individuals following ketogenic diets have very low fasting insulin levels, reflecting excellent insulin sensitivity.
Low insulin levels allow the body to mobilize fat efficiently for energy—but this may also increase lipoprotein transport.
Thyroid Signaling and Lipid Clearance
Another factor influencing LDL levels is thyroid signaling.
Thyroid hormone—especially the active hormone T3—regulates the number of LDL receptors in the liver.
These receptors help remove LDL particles from the bloodstream.
When thyroid signaling decreases, even slightly:
- LDL receptors decrease
- LDL particles remain in circulation longer
- LDL levels rise
Many lean ketogenic individuals display what could be described as energy-conserving thyroid physiology, where T3 levels fall slightly while metabolic efficiency improves.
This does not necessarily indicate thyroid disease—it may reflect metabolic adaptation to lower carbohydrate intake.
Why HDL Is High in LMHR Individuals
Another hallmark of the LMHR pattern is elevated HDL cholesterol.
HDL plays an important role in reverse cholesterol transport, helping move cholesterol from tissues back to the liver.
Higher HDL levels are often associated with:
- improved insulin sensitivity
- lower triglycerides
- better metabolic health
In LMHR individuals, HDL levels often rise alongside increased fat metabolism and improved metabolic flexibility.
Why Triglycerides Drop
Triglycerides typically fall when insulin resistance improves.
High triglycerides are often associated with:
- high carbohydrate intake
- insulin resistance
- metabolic syndrome
In contrast, low triglycerides often indicate:
- efficient fat metabolism
- stable blood sugar
- improved metabolic health
In many LMHR individuals, triglycerides drop significantly after adopting a ketogenic diet.
Why This Pattern Is Still Being Studied
The critical question researchers are now exploring is whether LDL behaves differently in the LMHR context.
Does high LDL in metabolically healthy individuals carry the same cardiovascular risk as high LDL in individuals with insulin resistance and metabolic syndrome?
Several studies are currently underway to better understand this question.
Researchers are examining factors such as:
- inflammatory markers
- coronary artery calcium scores
- lipoprotein particle characteristics
- metabolic health markers
These studies aim to determine whether the metabolic context surrounding LDL matters.
Evaluating Cardiovascular Risk More Broadly
For individuals who display the LMHR phenotype, many clinicians prefer to evaluate cardiovascular risk more comprehensively rather than focusing solely on LDL.
Additional markers often considered include:
• ApoB (lipoprotein particle count)
• Lipoprotein(a)
• hs-CRP (inflammation marker)
• fasting insulin
• coronary artery calcium score
These markers help provide a broader picture of cardiovascular risk.
Nutrient Status and Lipid Metabolism
Another factor sometimes overlooked in lipid metabolism is micronutrient sufficiency.
Certain nutrients support:
- thyroid hormone signaling
- mitochondrial respiration
- lipid metabolism in the liver
These include:
- vitamin A
- copper
- riboflavin
- choline
Traditional diets often included nutrient-dense organ meats such as liver, which provided these compounds in high concentrations.
Modern diets focused primarily on muscle meat may provide fewer of these nutrients.
Supporting micronutrient intake may help optimize metabolic pathways involved in lipid processing.
Metabolic Flexibility Matters
One of the key principles of metabolic health is flexibility—the body’s ability to efficiently use both fat and glucose as fuel when needed.
In some cases, individuals with the LMHR pattern may find that moderate adjustments in diet can influence lipid levels without abandoning metabolic health.
For example, some individuals see LDL levels decrease when they:
- reduce prolonged fasting
- increase protein intake
- modestly increase carbohydrate intake
The response varies widely between individuals, which is why personalized care is important.
A Systems Medicine Perspective
From a systems medicine perspective, LDL should be interpreted within the broader context of metabolism.
Key questions include:
- Is insulin resistance present?
- Are triglycerides elevated?
- Is inflammation high?
- Are metabolic markers improving?
In many individuals who adopt ketogenic diets, metabolic markers such as blood sugar, triglycerides, and inflammatory markers improve dramatically.
Understanding how LDL fits into that context remains an active area of research.
The Future of Lipid Science
The Lean Mass Hyper-Responder phenomenon highlights an important truth in medicine:
Human metabolism is complex.
Single biomarkers rarely tell the entire story.
As metabolic research continues to evolve, clinicians and researchers are increasingly recognizing the importance of examining the entire metabolic system, rather than focusing on one isolated marker.
The goal is not simply to normalize lab numbers but to understand how the body regulates energy, fuel transport, and metabolic resilience.
Final Thoughts
The Lean Mass Hyper-Responder phenotype represents a fascinating intersection of nutrition, metabolism, and lipid biology.
For some individuals, improving metabolic health through carbohydrate restriction may reveal a lipid pattern that challenges traditional assumptions.
Understanding this pattern requires careful evaluation, thoughtful clinical judgment, and ongoing research.
Ultimately, the goal is to support metabolic health while ensuring that cardiovascular risk is appropriately assessed and managed.
As with many aspects of medicine, the most effective approach is individualized care guided by a comprehensive understanding of physiology.