Mast Cell Activation Syndrome & Histamine Intolerance: Why Reactivity Develops—and How the Body Regains Stability
Mast Cell Activation Syndrome (MCAS) and histamine intolerance are often described as conditions that require lifelong avoidance, extreme restriction, or constant vigilance.
But that framing misses something essential.
Reactivity is not a character flaw of the immune system.
It is a context-dependent protective response—one that develops when the internal environment no longer feels predictable or safe.
Understanding why mast cells become reactive is the first step toward restoring tolerance.
Mast Cell Activation Syndrome: Environmental Sensors, Not Villains
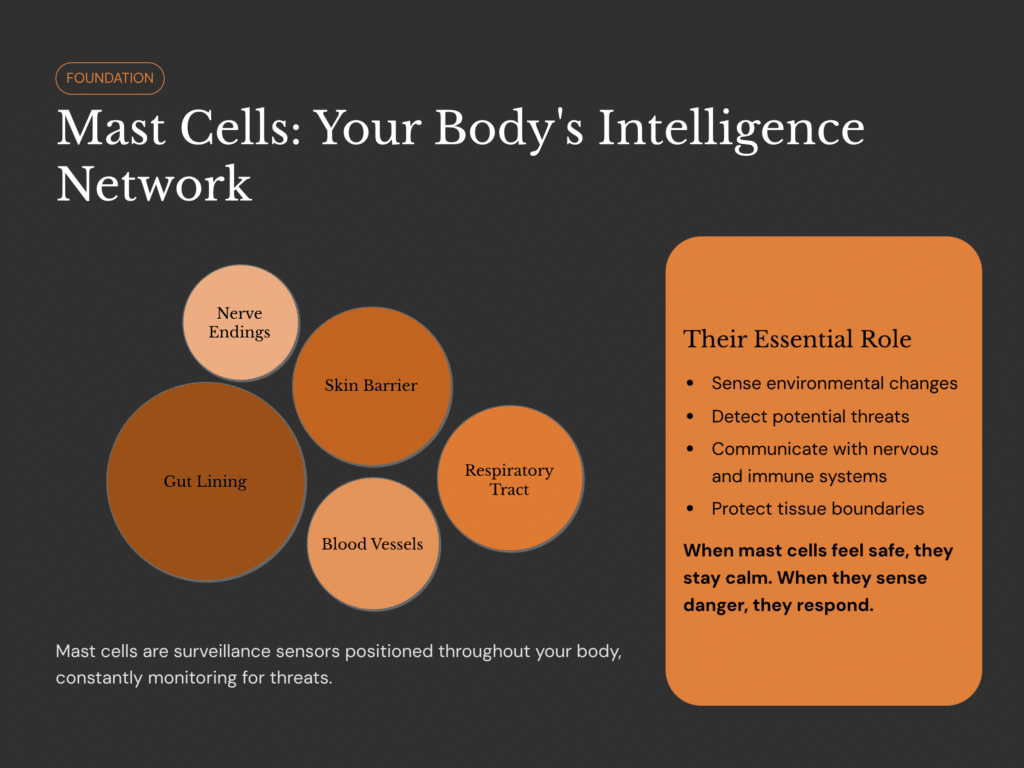
Mast cells are immune sentinels. They are designed to live at the body’s borders—where the internal world meets the external one.
You’ll find them concentrated in:
The gut lining
The skin
The respiratory tract
Around blood vessels and nerve endings
Their role is early detection and rapid communication. Mast cells sense environmental signals and relay information to both the immune system and the nervous system.
When conditions are stable, mast cells remain quiet.
When the terrain becomes unstable, they respond.
This is why mast cell reactivity is rarely random—and why it often fluctuates with stress, sleep, hormones, and environmental load.
Histamine Intolerance and MCAS Exist on a Spectrum
Although histamine intolerance and MCAS are often discussed as separate diagnoses, clinically they are better understood as patterns along a reactivity spectrum.
Histamine intolerance typically reflects:
Excess histamine load
Reduced clearance capacity
Gut inflammation or dysbiosis
Impaired DAO activity or nutrient insufficiency
This pattern is often situational and can improve when gut health and clearance pathways are restored.
MCAS reflects a deeper pattern of immune hypervigilance. Mast cells release mediators too easily, too frequently, and in response to lower-level stimuli.
This pattern frequently overlaps with:
Dysautonomia
Autoimmune activation
Chronic stress physiology
Mold or chemical exposure
Post-viral syndromes
Hormonal transitions, especially perimenopause and menopause
People may move along this spectrum over time depending on their internal and external load.
The Real Drivers of Mast Cell Reactivity
Mast cells become reactive when the body’s internal signaling systems lose coherence. Common upstream contributors include:
Gut Barrier Instability
The gut houses one of the largest mast cell populations in the body. When the gut lining is inflamed or permeable, mast cells are repeatedly stimulated, histamine clearance declines, and immune signaling becomes noisy.
Nervous System Dysregulation
Mast cells and the autonomic nervous system are in constant dialogue. When the nervous system remains in a state of threat or vigilance, mast cells follow suit. This explains the strong overlap between MCAS, anxiety, sleep disruption, and dysautonomia.
Environmental Burden
Mold, chemicals, and other environmental exposures can activate mast cells—especially when baseline resilience is already low. In many cases, food is not the primary driver; it is simply the most visible trigger.
Hormonal Shifts
Estrogen directly influences mast cell activity. Fluctuations during the menstrual cycle, perimenopause, and postmenopause can significantly lower the threshold for reactivity.
Metabolic and Immune Stress
Blood sugar instability, chronic inflammation, and immune activation reduce the system’s buffering capacity and amplify mast cell signaling.
Why Long-Term Avoidance Backfires
Low-histamine diets can be useful temporarily, particularly during periods of high reactivity. But when used as a long-term strategy, they often create unintended consequences.
Chronic restriction can:
Increase fear around food
Reduce nutrient diversity
Weaken gut resilience
Reinforce the belief that the body is fragile
The goal is not permanent avoidance.
The goal is restoring tolerance.
Tolerance returns when the systems that regulate mast cell behavior regain stability.
A Systems-Based Path to Calming Reactivity
From a systems medicine perspective, mast cell patterns do not improve through force or aggressive intervention.
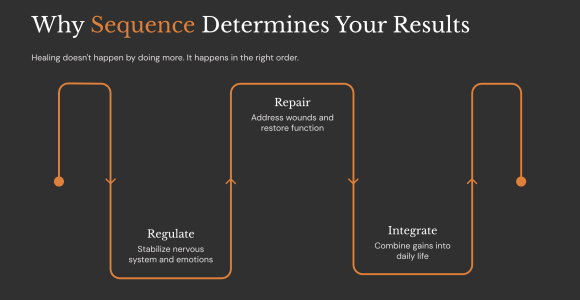
They improve through sequencing.
Stability comes first:
Nervous system regulation
Gentle containment rather than detox pressure
Blood sugar consistency
Reduction of inflammatory signaling
Only then does deeper repair become possible.
Many individuals with MCAS have been pushed too quickly—through aggressive detox protocols, excessive supplementation, or constant food experimentation. This often increases reactivity rather than resolving it.
The body calms when it feels resourced, supported, and safe.
What Healing Looks Like in Real Terms
Progress with MCAS and histamine patterns is rarely dramatic or instant.
Instead, it shows up as:
Fewer reactions overall
Reduced intensity when reactions occur
Faster recovery
Greater predictability and confidence
This is not symptom suppression.
It is restored regulation.
A Reframe Worth Holding
If there is one message worth carrying forward, it is this:
Your body is not attacking you.
It is protecting you—sometimes too diligently.
And protection can soften when the conditions that created vigilance begin to change.
That is the work of systems medicine: restoring communication, coherence, and trust inside the body.